Treating Depression
Recognise the signs and find fast-acting, effective treatments for sustainable recovery.

It is common to experience mood swings and short-term negative emotions as a response to life challenges. However, if you experience persistent feelings of sadness that interfere with your day-to-day life in it may be a sign of something more serious.
A depressive episode is characterized by ongoing symptoms, lasting a minimum of two weeks, a daily deflected mood and a diminished enjoyment or interest in everyday activities.
1 in 16 people in Australia are affected by depression each year. While it is a serious medical condition that affects both mental and physical health, it can be treated with the right clinical support.
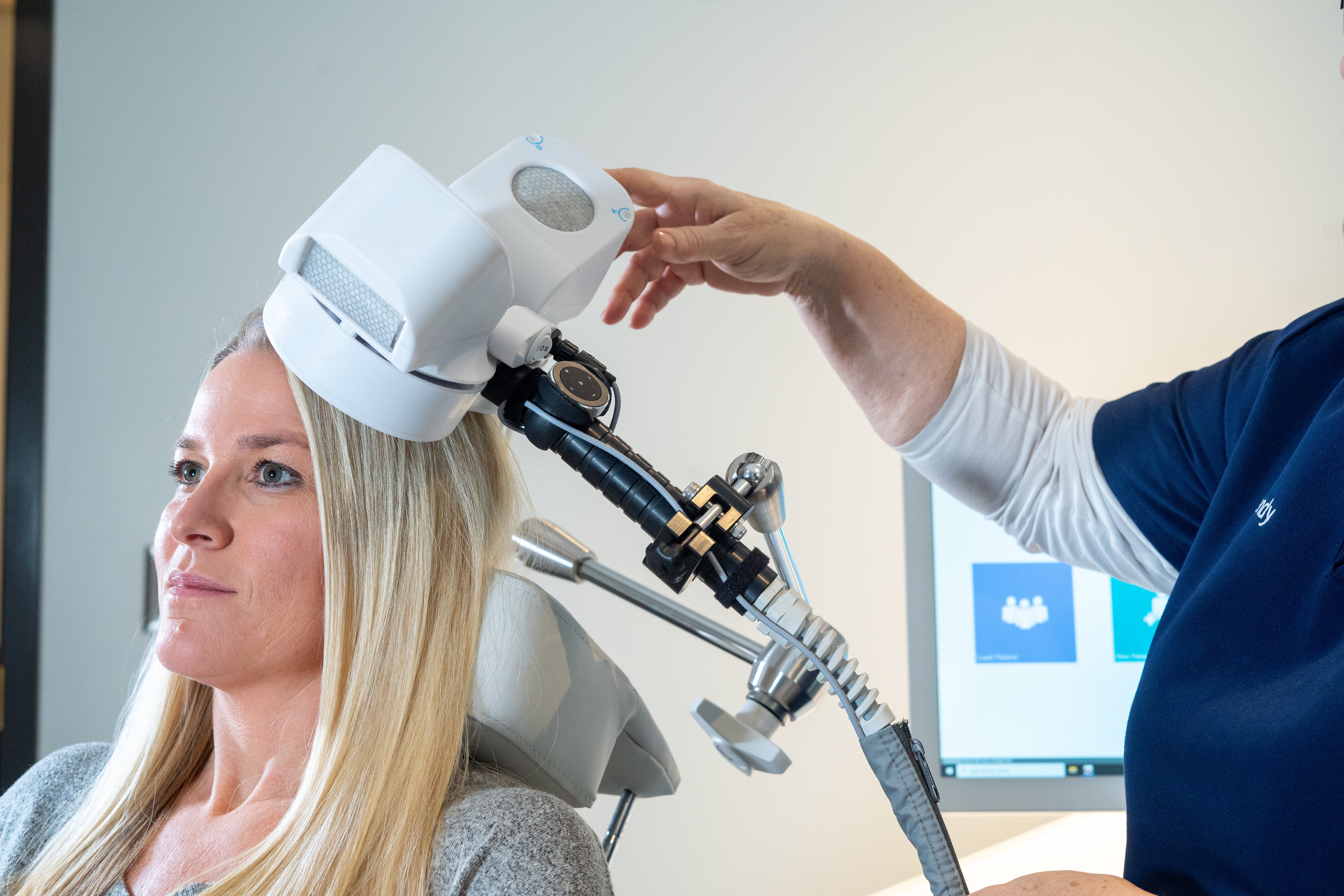
Medicare rebates are available for TMS therapy, for those with depression who have not responded to antidepressant medications or psychotherapy.
Causes of Depression
Depression is rarely caused by one single factor. In most cases, it is the result of a complex combination of biological, psychological, and social factors including:
- Life events
Adverse life events like bereavement or unemployment make you more likely to develop depression. - Family history
Those with close relatives who have experienced depression are more likely to develop the condition. - Medical conditions
Certain illnesses like cardiovascular disease, diabetes, insomnia or chronic pain can contribute to depression as can certain medications. - Substance use
A history of substance or alcohol misuse can affect your risk. - Individual characteristics
Personality traits such as low-self-esteem, sensitivity to criticism and perfectionism are all correlated with a higher chance of depression.
Symptoms of Depression
Common symptoms and feelings associated with depression include:
Treatment for Depression
Antidepressant Medications
The antidepressant medications used today have been available since the 1950s. They have become a mainstay treatment for depression, however professional opinions on their effectiveness vary. Medications are shown to help with moderate, severe, and chronic depression.
Antidepressants work by relieving the symptoms of depression to help the patient feel a returned sense of emotional stability. They may also be used to prevent a relapse of depressive symptoms.
Like many oral medications, antidepressants can have side effects, which are often more noticeable at the beginning of the treatment. You may experience headaches, dizziness, dry mouth, weight gain, loss of libido and other side effects depending on the type of antidepressant.
At neurocare we are exploring the use of QEEG, a brain mapping technique used in our clinics, to help predict if a patient will respond to certain antidepressant medication. This may allow psychiatrists to better target and personalise treatment for depression.

Psychotherapy
Psychotherapy – also known as talk therapy - can be an effective treatment for depression. Psychotherapy can be delivered by a trained Psychologist, Psychiatrist, or other Medical Doctor. Cognitive-behavioural therapy (CBT) and interpersonal therapy have shown good results, but there are other evidence-based forms of psychotherapy that may be recommended and tailored to you.
Psychotherapy can help you adjust to difficult circumstances and build awareness of thinking and behaviour. Together with your clinician, you will learn to identify negative behaviours and beliefs and workshop alternative perspectives and coping strategies.
For some patients who may need more acute intervention for Depression, Psychotherapy on its own may not be as effective or may take several months or years to reach an improved mindset. Often this bears a large and ongoing out-of-pocket expense to the patient. For faster effects, Psychotherapy can be integrated with other treatments like medication or Neurostimulation techniques like TMS. The dual effect can help boost progress and recovery in a shorter time frame.
Learn more about Psychotherapy
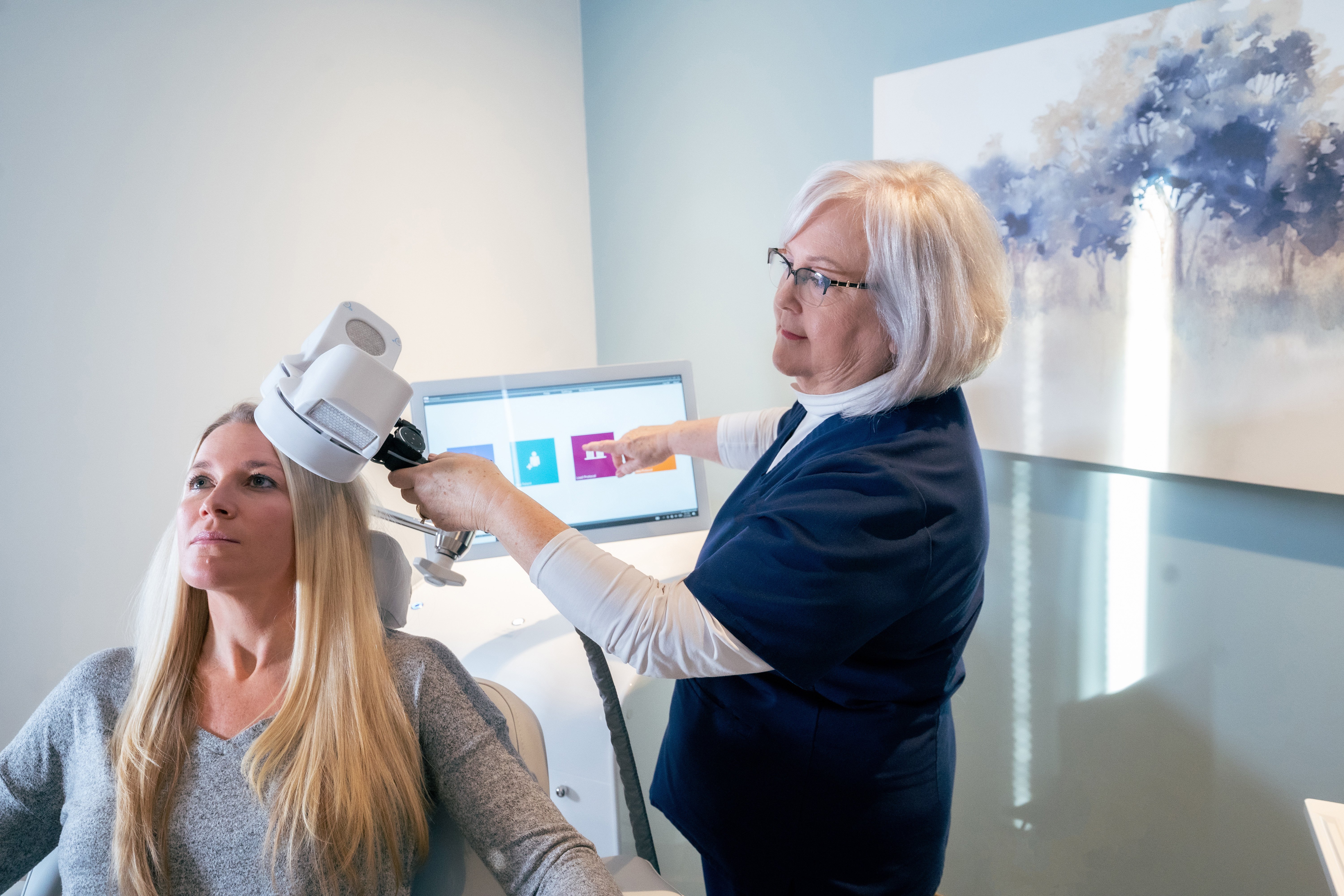
Transcranial Magnetic Stimulation (TMS)
TMS is a fast-acting and sustainable treatment that works by delivering magnetic pulses to alter the activity within the brain networks that regulate our mood.
TMS is RANZCP endorsed for the treatment of depression. It is a fast-acting and sustainable therapy with minimal side effects.
neurocare uses an evidence-based approach which combines TMS with Psychotherapy to maximise the brain's natural ability to change and recover.
Research into personalised treatment approaches has shown that patients have a higher chance achieving remission from depression with our combined approach when compared to medication, psychotherapy alone or TMS monotherapy.
How TMS helps with Depression
TMS is a well-tolerated and proven method to treat Depression, even in patients who have not responded to other forms of therapy. The majority of patients (66%) respond well to this treatment when it is combined with psychotherapy (Donse et al. 2017).
Not sure if our services are right for you?




