Sleep Assessments
Track your sleep and wake routine and exposure to light through non-invasive Actigraphy technology.

Straight to:
Sleep issues underlie a wide range of mental health problems. They can cause or exacerbate symptoms in ADHD, depression, OCD, anxiety and general learning, behavioural or mood disorders.
Assessment and treatment of sleep problems can significantly improve the outcome of other therapies, but obtaining an objective picture of your sleep patterns can be difficult. An Actigraphy assessment can help.
How does an Actigraphy Assessment work?

An actigraphy assessment involves wearing a tracking wristband over seven days to gather a continuous stream of data on your sleep/wake behaviour. It also records other environmental factors such as blue light exposure, exercise, sleep onset latency, bedroom and body temperature.
The results will provide your clinician with accurate insights to help them identify any underlying sleep issues your may have or rule them out as a contributing factor to your symptoms.
The impact of blue light on sleep
Blue spectrum light plays an important role in our sleep-wake cycle. Our circadian rhythm (or “internal clock”) is regulated by the absorption of blue light in the melanopsin receptors of the eyes.
Modern display devices (TVs, phones, tablets and laptops) and LED and fluorescent light bulbs emit a high spectrum blue light. Overexposure to blue spectrum light in the evenings and especially before bedtime stops our bodies from releasing sleep-inducing melatonin. This can have a big effect on our quality of sleep and duration of sleep. When we do not have good sleep this can affect our mood and attention.
.png?width=8164&name=sun%20moon%20clock%20(2).png)
What Actigraphy Sleep Assessments show
Sleep routine
An Actigraphy wristband is usually worn over a 7 day period. The report that is generated after this period will objectively track your sleep habits, including when you are going to bed and waking up.
Light exposure
Exposure to blue spectrum light throughout the day and evening can affect our body's ability to produce melatonin and fall asleep. Actigraphy will track your exposure to blue and other spectrums of light to identify any concerns.
Restlessness
Actigraphy can detect periods of restlessness during the night including how frequently you are waking up and any periods of interrupted sleep.
Activity
Like other activity trackers, Actigraphy also includes accelerometer technology which picks up your level of activity throughout the day. Those with lower activity levels are more likely to have trouble sleeping.
Frequently Asked Questions
-
Your sleep/wake behaviour can provide important insights regardless of whether you have reported a sleep problem. Clients who report difficulty with mood or attention quite frequently have underlying sleep issues. With Actigraphy, we can understand the extent of any problem or rule it out as a contributor to your symptoms or feelings.
-
Wear the wristband for 7 days to allow it to collect continuous data on your activity, and sleep/wake behaviour. You simply need to push the blue button on the wristband when you intend to go to sleep and again when you wake up. This will make a marker on your “Actigraphy chart”. While the Actigraphy data will show us when you likely went to sleep and when you wake up, pressing this button this allow us to cross-check the data.
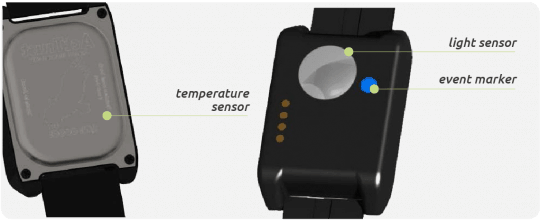
-
An Actigraphy tracker has a light sensor to measure your exposure to blue light in the evenings.
-
Smartphones, tablets, desktop computers, LED and fluorescent lamps emit a high spectrum of blue light which the human brain more naturally needs to be exposed to during daylight hours. Overexposure to blue spectrum light in the evenings, especially before bedtime, counteracts the body’s release of sleep-inducing melatonin. These impact sleep quality and duration, affecting mood and attention levels.
By tracking blue light exposure against your sleep and wake patterns, we can see if the light in your environment affects your sleep.
-
Visualising our sleep/wake patterns and general activity patterns can be an eye-opening experience. There are different types of sleep problems, for example, people who show lengths of restlessness before falling asleep (called “sleep onset latency”), or people who fall asleep but appear restless during the night. These differences may explain what we see in the QEEG assessment.
Investigating your exposure to blue light flags potential sources of blue light (e.g. too much blue light in your bedroom) as well as identifying any unhelpful patterns of behaviour. This allows you to introduce new strategies and behaviours which can help you achieve improved sleep outcomes.
Not sure if our services are right for you?




