In which countries is TMS therapy insured?
June 16, 2023 - neurocare group
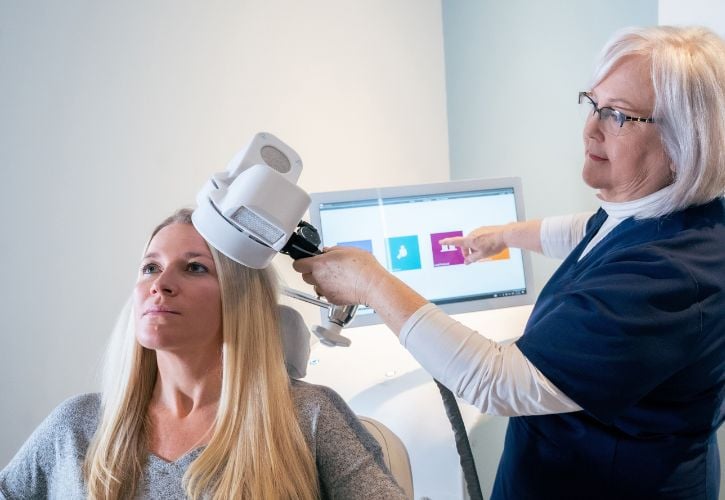
TMS therapy, or (repetitive) transcranial magnetic stimulation therapy, is a non-invasive treatment gaining attention for being a safe and fast-acting alternative treatment for depression. Research has shown that TMS therapy, also known as rTMS, may be an effective option for alleviating symptoms of depression in a relatively short amount of time. Typically, patients attend at least two sessions per week for a duration of 20 to 30 sessions.
To undergo TMS therapy, patients require the expertise of trained professionals who operate specialized equipment. Patients and their families may have questions regarding the cost of completing a TMS therapy program, and whether health insurance can cover some or all of the treatment expenses due to the multiple sessions required.
The reimbursement coverage for TMS therapy by private or public insurance providers can vary depending on the country and specific insurance policies. It is important to take into account additional factors when determining eligibility for insurance coverage and obtaining a referral for TMS therapy treatment, such as getting an assessment and diagnosis from a trained professional.
TMS is already reimbursed in several countries. Here we have outlined which countries offer financial support for TMS therapy in the treatment of depression, and what other important factors you should take into account.
Reimbursement of TMS therapy in the United States
In the United States, TMS therapy is covered by the majority of private insurance providers, including Medicare and some Medicaid programs. However, coverage may vary depending on the specific insurance plan and individual circumstances.
To access TMS therapy in the United States for the treatment of depression, a prior-authorization process is generally required by the insurance company. This process will try to factor in, for example, whether or not the client has not found benefit from other first-line interventions . It is advisable to check with your insurance provider to determine the extent of coverage and any associated requirements.
For more information on TMS Therapy in the United States visit www.neurocarecentersofamerica.com
Reimbursement of TMS Therapy in Australia
Since 2021, TMS therapy has been included in the Medicare Benefits Schedule (MBS) in Australia. This means that patients diagnosed with Major Depression can receive a subsidy to cover the cost of multiple rTMS treatment sessions. To qualify for the subsidy, patients need to have a diagnosis of a major depressive episode and have not responded to two or more antidepressant medications.
For more information on TMS therapy in Australia, visit www.neurocareclinics.com.au
Reimbursement of TMS therapy in The Netherlands
In 2017 the Dutch Health Authority advised health insurance companies to incorporate TMS therapy for the treatment of Treatment Resistant Depression. Patients in The Netherlands who are insured with providers such as CZ, VGZ, Menzis, Zorg en Zekerheid, DSW and Zilveren Kruis, for example, may be eligible to receive a subsidy for TMS treatment sessions.
Only patients who have tried two or more previous therapies, for example, psychotherapy or pharmacotherapy, and have not had a sufficient response to this therapy, would be eligible to receive a subsidy for treatment with TMS therapy.
For more information on TMS Therapy in the Netherlands, visit: www.neurocaregroup.com/nl/
These examples are not exhaustive, and reimbursement coverage for TMS therapy may be subject to change. It is crucial to check with specific insurance providers and healthcare authorities in your country or region to obtain accurate and up-to-date information regarding reimbursement for TMS therapy.






